Eczema
Eczema (also called atopic eczema or atopic dermatitis) is a very common dry skin condition. It affects about 1in 5 babies and children in the UK. Eczema often appears in the first few months of life. Eczema usually improves in most children as they get older, but some children with more severe eczema may continue to have eczema into adult life.
Eczema can cause the skin to become itchy, dry, cracked and sore. Sometimes, children with eczema make may have periods where the eczema becomes more severe (flare ups).
Many things, called “trigger factors” can make the eczema worse. These include:
-
Irritants such as soap, clothing (wool, polyester), cigarette smoke, chlorine in swimming pools
-
Changes in the climate such as drier air or temperature (too cold or too hot)
-
Environmental allergens such as house dust mite and moulds
-
Viral illnesses
-
Hormone changes
-
Stress and anxiety
-
Rarely foods
-
Immediate reactions (less than 1 hour) after eating.
-
Delayed reactions (4 to 6 hours) after eating with a flare of eczema.
-
The National Eczema Society has more information about household triggers and how to manage them
There is currently no cure for eczema, however avoiding trigger factors and using of moisturisers 3 to 4 times a day can help keep it under control. Your local community pharmacist or GP can advice you if other treatment for eczema is needed.
The exact cause of eczema is unknown. It is not down to one thing. Atopic eczema often occurs in people who get allergies. “Atopic” means sensitivity to allergens. This type of eczema can run in families, and often develops with other conditions like asthma and hay fever.
If you are worried that the eczema rash looks different to normal please see our page on rashes for advice on where to seek help.
How to tell it’s eczema?
Eczema in babies often appears at between 3-6 months of age. It can develop anytime after birth or in childhood.
The main features of eczema are:
-
Intense itch
-
Dry skin
-
Rash
-
Redness
-
Inflammation
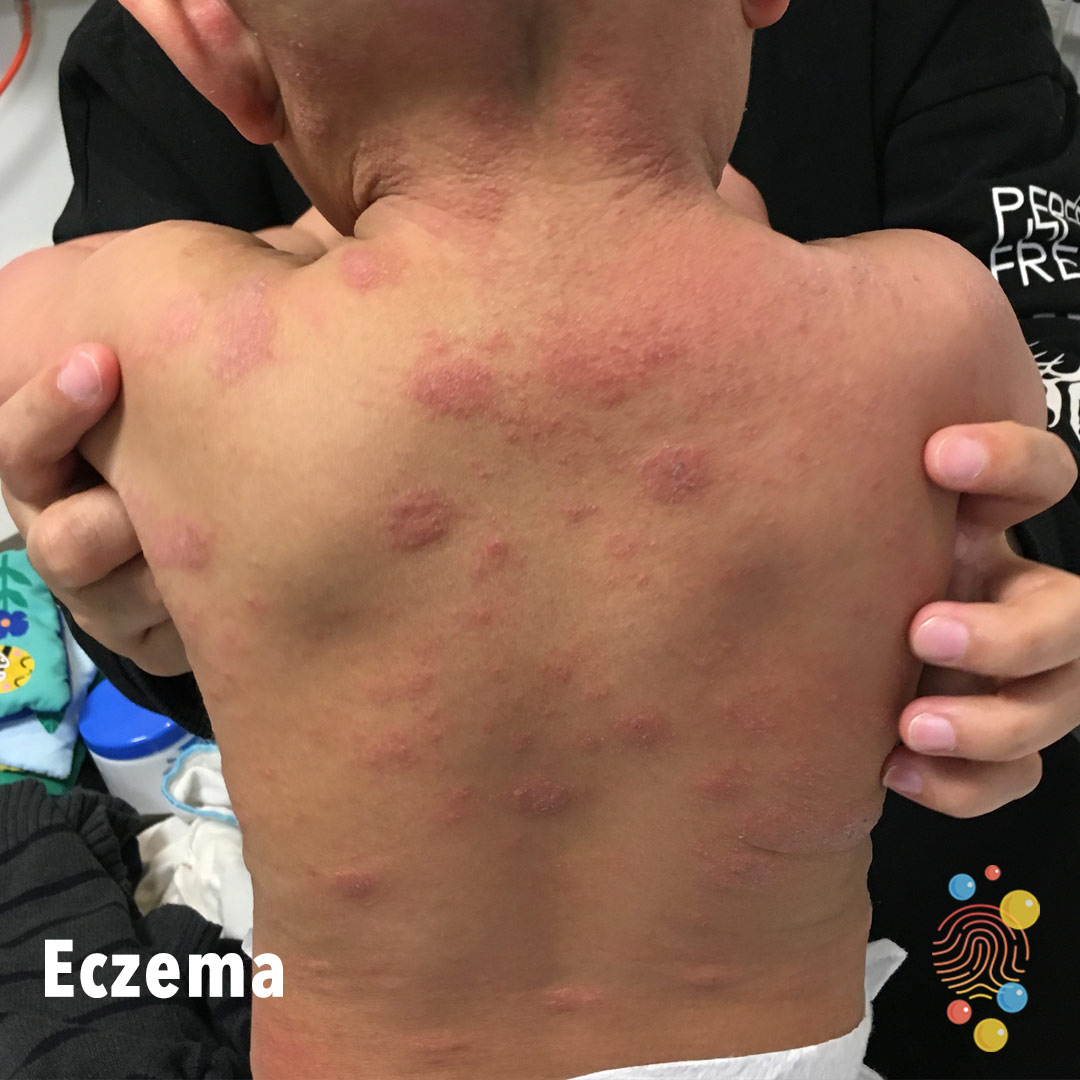
In infants and babies, eczema affects the face, scalp and body. It does not usually affect the nappy area. As your child grows older the pattern of eczema changes. It affects the skin behind the elbow and the knee. In some children it affects the whole body.
In children of Asian, black Caribbean or black African ethnic groups, eczema can affect different places including the front surface of the knee or wrist. It can also look different with the skin being bumpy and slightly darker instead of red
It is important to be aware of and look for signs of worsening eczema
Recognise a flare: A ‘flare’ is a worsening of the eczema. Skin may become red, sore, (more)itchy, crack or bleed
Recognise infected eczema: If skin suddenly worsens, weeps fluid or crusts it could be infected and your child may need antibiotics. Seek urgent advice if your child is unwell or the infection is widespread.
Blisters or cold sores need urgent antiviral treatment. See your GP or seek medical advice the same day.
Food allergy: this is rare. Consider food allergy if eczema started as a baby. It is not usually the cause of eczema in older children.
How to treat eczema
Treatment of eczema can help reduce symptoms. Most children’s eczema improves over time. Severe eczema can have significant impact on daily life. Eczema has an increased risk of skin infections.
Top Tips
-
Moisturise every day, even when the skin is clear of eczema
-
Apply moisturiser using downward strokes. Do not rub it in
-
Do an extra rinse when washing clothes
-
Wear soft, comfortable, loose clothing
-
Keep fingernails short to prevent scratching
Emollients
-
Emollients are moisturisers that soften the skin. It is okay to try different emollients. Talk to your GP or nurse if you do not like one you have been given
-
Expect to use large amounts. A large tub (250 to 500 g) per week
-
Use everyday, all over
-
You may need to change emollient type if one does not work
-
Emollients form a protective barrier on the skin
-
Emollients are best used few minutes after a warm bath, while the skin is still slightly damp
-
Emollients are safe so they can be used as many times a day as needed
-
Use at least 2 times a day when skin clear but increase to 4 to 6 times a day during flare ups or when the skin looks dry
-
Do not put hands in tubs of emollients as these can introduce “bugs” easily. This is a common reason for repeated skin infections in eczema. Use a clean spoon or spatula to get emollients out of the tub
-
For school and for older children and young people emollients with pumps may be better
-
Apply in direction of hair growth. This reduces the chance of infection
-
Fire hazard. Most eczema treatments contain paraffin and are flammable
Bathing & Showering
-
Avoid Bubble baths and perfumed products (some of the eczema bath products can provide bubbles if put in running water)
-
Use your moisturiser (emollient) or a soap free wash to cleanse skin. Soap or soap based products can dry the skin.
-
Bath water should be tepid or lukewarm as heat is a common eczema trigger
-
Skin should be patted dry after bath
Topical (On Skin) Steroids
-
Steroid creams and ointments are treatments for flare ups of eczema and help heal the skin. Steroids come in different strength from mild to strong steroids.
-
Steroids are safe when used in short courses as advised by your doctor. When applying it is important to apply sparingly to the skin so that skin glistens.
-
Use topical steroids once a day to eczema that is red and itchy. Stop when no longer red and itchy and restart if eczema comes back.
-
Leave a gap of 20 mins between applying your emollient and steroid. This is so that the topical steroid is not made less effective by the emollient.
See your doctor if:
- Eczema is infected. It may be pustules, blisters, painful, weeping fluid. Antibiotics may be needed.
- Eczema is not going away with regular daily use of topical steroids for 2 weeks.
- Eczema is causing waking at night, missing school or mood problems.
Helpful resources
Allergy Care Pathway Itchy Sneezy Wheezy Project - Eczema Videos
Where should you seek help?
- If it is non-urgent speak to your local pharmacist or health visitor
- If your child has any of the above features, urgently see your GP. For an urgent out-of-hours GP appointment, call NHS 111
- You should only call 999 or go to your nearest A&E department in critical or life threatening situations
For wear and tear, minor trips and everything in between.
Self-care
You can treat your child's very minor illnesses and injuries at home.
Some illnesses can be treated in your own home with support and advice from the services listed when required, using the recommended medicines and getting plenty of rest.
Sound advice
Children can recover from illness quickly but also can become more poorly quickly; it is important to seek further advice if a child's condition gets worse.
For information on common childhood illnesses go to What is wrong with my child?
Pharmacists are experts in many aspects of healthcare and can offer advice on a wide range of long-term conditions and common illnesses such as coughs, colds and stomach upsets. You don’t need an appointment and many have private consultation areas, so they are a good first port of call. Your pharmacist will say if you need further medical attention.
Sound advice
- Visit a pharmacy if your child is ill, but does not need to see a GP.
- Remember that if your child's condition gets worse, you should seek further medical advice immediately.
- Help your child to understand - watch this video with them about going to the pharmacy.
For information on common childhood illnesses go to What is wrong with my child?
Health visitors are nurses or midwives who are passionate about promoting healthy lifestyles and preventing illness through the delivery of the Healthy Child Programme. They work with you through your pregnancy up until your child is ready to start school.
Health Visitors can also make referrals for you to other health professionals for example hearing or vision concerns or to the Community Paediatricians or to the child and adolescent mental health services.
Contact them by phoning your Health Visitor Team or local Children’s Centre.
Sound advice
Health visitors also provide advice, support and guidance in caring for your child, including:
- Breastfeeding, weaning and healthy eating
- Exercise, hygiene and safety
- Your child’s growth and development
- Emotional health and wellbeing, including postnatal depression
- Safety in the home
- Stopping smoking
- Contraception and sexual health
- Sleep and behaviour management (including temper tantrums!)
- Toilet training
- Minor illnesses
For more information watch the video: What does a health visitor do?
School nurses care for children and young people, aged 5-19, and their families, to ensure their health needs are supported within their school and community. They work closely with education staff and other agencies to support parents, carers and the children and young people, with physical and/or emotional health needs.
Primary and secondary schools have an allocated school nurse – telephone your child’s school to ask for the contact details of your named school nurse.
There is also a specialist nurse who works with families who choose to educate their children at home.
Sound Advice
Before your child starts school your health visitor will meet with the school nursing team to transfer their care to the school nursing service. The school nursing team consists of a school nursing lead, specialist public health practitioners and school health staff nurses.
They all have a role in preventing disease and promoting health and wellbeing, by:-
- encouraging healthier lifestyles
- offering immunisations
- giving information, advice and support to children, young people and their families
- supporting children with complex health needs
Each member of the team has links with many other professionals who also work with children including community paediatricians, child and adolescent mental health teams, health visitors and speech and language therapists. The school health nursing service also forms part of the multi-agency services for children, young people and families where there are child protection or safeguarding issues.
If you’re not sure which NHS service you need, call 111. An adviser will ask you questions to assess your symptoms and then give you the advice you need, or direct you straightaway to the best service for you in your area.
Sound advice
Use NHS 111 if you are unsure what to do next, have any questions about a condition or treatment or require information about local health services.
For information on common childhood illnesses go to What is wrong with my child?
A&E departments provide vital care for life-threatening emergencies, such as loss of consciousness, suspected heart attacks, breathing difficulties, or severe bleeding that cannot be stopped. If you’re not sure it’s an emergency, call 111 for advice.




